Health & Wellbeing
Your Eyes & Voice Hold Parkinson's Secret, Years Before Doctors See It.
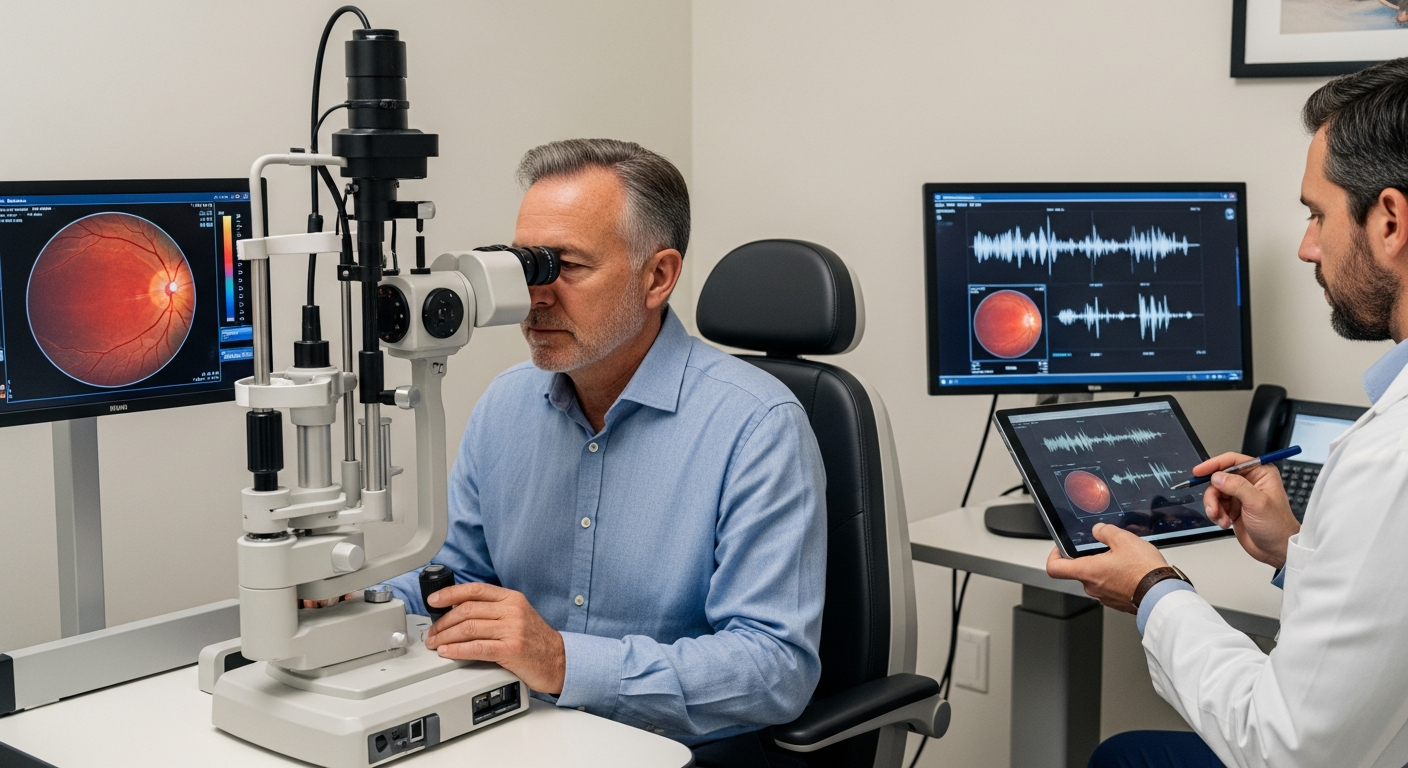
For decades, diagnosing Parkinson's disease (PD) has been a race against time, often confirmed only after irreversible motor symptoms emerge, leaving patients years behind on potential interventions. But a revolutionary shift is underway: Artificial Intelligence is now unmasking the silent signals of Parkinson's in places doctors rarely thought to look—our eyes and voices—up to seven years before clinical diagnosis. This isn't just an incremental improvement; it's a profound redefinition of early detection, poised to transform how we approach one of the fastest-growing neurological conditions globally.
Imagine an ordinary eye exam revealing your future neurological health. This is rapidly becoming a reality. Researchers from Moorfields Eye Hospital and UCL Institute of Ophthalmology, utilizing AI to analyze hundreds of thousands of retinal scans, have identified subtle 'retinal markers' that indicate Parkinson's disease up to seven years before symptoms appear. This groundbreaking work, published in 2023 and further explored in 2025-2026, represents the largest study to date on retinal imaging in Parkinson's.
The retina, an extension of the central nervous system, offers a non-invasive window into brain health. AI algorithms, particularly convolutional neural networks, are now adept at spotting minute changes in retinal structures, such as thinning of the retinal nerve fiber layer, altered vascular patterns, and even the loss of dopaminergic cells—all critical indicators previously overlooked by the human eye.
Beyond static images, your eye movements themselves betray early signs. Companies like Neuralight are leveraging AI to track nuanced eye movement abnormalities (oculometrics) through facial videos captured with standard webcams. These computer-based tests, more sensitive than traditional neurological assessments, can monitor disease progression and even aid in diagnosis by detecting slower, less accurate eye movements characteristic of early PD. This emerging field, dubbed 'oculomics,' is also showing promise for other neurodegenerative conditions like Alzheimer's and multiple sclerosis.
Equally astonishing is AI's ability to extract diagnostic insights from the subtle nuances of human speech. Scientists at the University of Rochester have developed an AI-powered screening tool that analyzes speech patterns to detect Parkinson's with remarkable accuracy, achieving nearly 86% success in identifying the disease across diverse demographics. Another study from March 2026 demonstrated ensemble machine learning models explaining 91% of variance in motor Unified Parkinson's Disease Rating Scale (UPDRS) scores by analyzing dysphonia measures from sustained phonation.
Speech impairments, or hypokinetic dysarthria, often manifest early in Parkinson's, long before noticeable motor tremors. AI models can identify subtle, non-linear patterns in high-dimensional speech data that are virtually undetectable to the human ear, such as micro-pauses, changes in pitch stability (jitter), amplitude (shimmer), and overall voice quality. This non-invasive approach is not only scalable and cost-effective but also holds immense potential for at-home monitoring via widely used speech-based interfaces like smart speakers, democratizing access to early screening, especially in underserved regions.
The significance of these breakthroughs cannot be overstated. Parkinson's disease affects approximately 8.5 million individuals worldwide, a number projected to double by 2040. Currently, diagnosis typically occurs when 60-80% of dopamine-producing neurons are already lost, making effective intervention challenging. AI's capacity to identify PD in its prodromal phase—years before motor symptoms—opens a critical window for neuroprotective treatments and lifestyle changes that could slow or even alter disease progression.
The real power lies in multimodal AI approaches, combining these subtle markers with other data. Researchers at Lund University in Sweden, for instance, developed an AI model in March 2026 that can detect five different neurodegenerative conditions, including Parkinson's, from a *single blood sample* by analyzing protein patterns across a database of 17,000 individuals. This 'joint learning' approach identifies general patterns of brain degeneration, revealing biological subtypes that traditional clinical diagnoses often miss, challenging the 'one-size-fits-all' treatment paradigm.
Similarly, the University of Florida's AIDP (Automated Imaging Differentiation for Parkinsonism) software, developed in collaboration with 21 sites, uses AI to analyze diffusion-weighted MRI scans, achieving over 96% precision in differentiating Parkinson's from similar movement disorders, significantly reducing misdiagnosis rates which can be as high as 25-50%.
This diagnostic revolution extends far beyond individual patient care, impacting several industries:
* Pharmaceutical R&D: Early, precise identification of at-risk individuals is a game-changer for drug development. Clinical trials can recruit patients in the prodromal stage, testing neuroprotective therapies before significant neuronal damage occurs, dramatically increasing the chances of success for disease-modifying drugs.
* Personalized Medicine & Longevity: The ability to predict disease trajectory and identify biological subtypes allows for truly personalized treatment plans, optimizing interventions for each individual's unique progression. This aligns with the broader longevity trend, where proactive health management is paramount.
* Healthcare Economics & Insurance: Early detection can shift the focus from costly late-stage symptomatic management to more affordable preventative or disease-slowing interventions, potentially reducing the long-term economic burden of neurodegenerative diseases. Insurance models may evolve to incentivize early, AI-driven screening.
* Technology & Consumer Health: The integration of AI diagnostics into everyday devices (webcams, smartphones, smart speakers) blurs the lines between consumer tech and medical screening, making health monitoring more accessible and ubiquitous.
Keep an eye on the rapid clinical validation and regulatory approvals (e.g., FDA) for these AI-powered diagnostic tools. Moorfields Eye Hospital and UCL are actively working towards making retinal scans a pre-screening tool. The University of Florida team is seeking FDA approval for their AIDP software. Expect to see more multi-modal platforms emerge, combining genetic, imaging, speech, and oculometric data for even higher predictive accuracy. The development of user-friendly, standalone AI applications for prognostication and personalized management, like the mAIcompass project, will also be critical for clinical implementation.
For individuals, this heralds a future where routine check-ups might include quick, AI-enhanced assessments of your eyes and voice, offering unprecedented insights into your neurological health. The goal is no longer just treating symptoms, but predicting and preventing, maximizing healthy years. It's time to pay attention to the subtle messages your body is sending, because AI is finally learning to listen.
The Unseen Clues in Your Gaze
Imagine an ordinary eye exam revealing your future neurological health. This is rapidly becoming a reality. Researchers from Moorfields Eye Hospital and UCL Institute of Ophthalmology, utilizing AI to analyze hundreds of thousands of retinal scans, have identified subtle 'retinal markers' that indicate Parkinson's disease up to seven years before symptoms appear. This groundbreaking work, published in 2023 and further explored in 2025-2026, represents the largest study to date on retinal imaging in Parkinson's.
The retina, an extension of the central nervous system, offers a non-invasive window into brain health. AI algorithms, particularly convolutional neural networks, are now adept at spotting minute changes in retinal structures, such as thinning of the retinal nerve fiber layer, altered vascular patterns, and even the loss of dopaminergic cells—all critical indicators previously overlooked by the human eye.
Beyond static images, your eye movements themselves betray early signs. Companies like Neuralight are leveraging AI to track nuanced eye movement abnormalities (oculometrics) through facial videos captured with standard webcams. These computer-based tests, more sensitive than traditional neurological assessments, can monitor disease progression and even aid in diagnosis by detecting slower, less accurate eye movements characteristic of early PD. This emerging field, dubbed 'oculomics,' is also showing promise for other neurodegenerative conditions like Alzheimer's and multiple sclerosis.
Your Voice: A Digital Biomarker
Equally astonishing is AI's ability to extract diagnostic insights from the subtle nuances of human speech. Scientists at the University of Rochester have developed an AI-powered screening tool that analyzes speech patterns to detect Parkinson's with remarkable accuracy, achieving nearly 86% success in identifying the disease across diverse demographics. Another study from March 2026 demonstrated ensemble machine learning models explaining 91% of variance in motor Unified Parkinson's Disease Rating Scale (UPDRS) scores by analyzing dysphonia measures from sustained phonation.
Speech impairments, or hypokinetic dysarthria, often manifest early in Parkinson's, long before noticeable motor tremors. AI models can identify subtle, non-linear patterns in high-dimensional speech data that are virtually undetectable to the human ear, such as micro-pauses, changes in pitch stability (jitter), amplitude (shimmer), and overall voice quality. This non-invasive approach is not only scalable and cost-effective but also holds immense potential for at-home monitoring via widely used speech-based interfaces like smart speakers, democratizing access to early screening, especially in underserved regions.
The Urgency of Early Detection: A Multimodal Revolution
The significance of these breakthroughs cannot be overstated. Parkinson's disease affects approximately 8.5 million individuals worldwide, a number projected to double by 2040. Currently, diagnosis typically occurs when 60-80% of dopamine-producing neurons are already lost, making effective intervention challenging. AI's capacity to identify PD in its prodromal phase—years before motor symptoms—opens a critical window for neuroprotective treatments and lifestyle changes that could slow or even alter disease progression.
The real power lies in multimodal AI approaches, combining these subtle markers with other data. Researchers at Lund University in Sweden, for instance, developed an AI model in March 2026 that can detect five different neurodegenerative conditions, including Parkinson's, from a *single blood sample* by analyzing protein patterns across a database of 17,000 individuals. This 'joint learning' approach identifies general patterns of brain degeneration, revealing biological subtypes that traditional clinical diagnoses often miss, challenging the 'one-size-fits-all' treatment paradigm.
Similarly, the University of Florida's AIDP (Automated Imaging Differentiation for Parkinsonism) software, developed in collaboration with 21 sites, uses AI to analyze diffusion-weighted MRI scans, achieving over 96% precision in differentiating Parkinson's from similar movement disorders, significantly reducing misdiagnosis rates which can be as high as 25-50%.
Beyond Healthcare: Economic & Industry Ripples
This diagnostic revolution extends far beyond individual patient care, impacting several industries:
* Pharmaceutical R&D: Early, precise identification of at-risk individuals is a game-changer for drug development. Clinical trials can recruit patients in the prodromal stage, testing neuroprotective therapies before significant neuronal damage occurs, dramatically increasing the chances of success for disease-modifying drugs.
* Personalized Medicine & Longevity: The ability to predict disease trajectory and identify biological subtypes allows for truly personalized treatment plans, optimizing interventions for each individual's unique progression. This aligns with the broader longevity trend, where proactive health management is paramount.
* Healthcare Economics & Insurance: Early detection can shift the focus from costly late-stage symptomatic management to more affordable preventative or disease-slowing interventions, potentially reducing the long-term economic burden of neurodegenerative diseases. Insurance models may evolve to incentivize early, AI-driven screening.
* Technology & Consumer Health: The integration of AI diagnostics into everyday devices (webcams, smartphones, smart speakers) blurs the lines between consumer tech and medical screening, making health monitoring more accessible and ubiquitous.
What to Watch
Keep an eye on the rapid clinical validation and regulatory approvals (e.g., FDA) for these AI-powered diagnostic tools. Moorfields Eye Hospital and UCL are actively working towards making retinal scans a pre-screening tool. The University of Florida team is seeking FDA approval for their AIDP software. Expect to see more multi-modal platforms emerge, combining genetic, imaging, speech, and oculometric data for even higher predictive accuracy. The development of user-friendly, standalone AI applications for prognostication and personalized management, like the mAIcompass project, will also be critical for clinical implementation.
For individuals, this heralds a future where routine check-ups might include quick, AI-enhanced assessments of your eyes and voice, offering unprecedented insights into your neurological health. The goal is no longer just treating symptoms, but predicting and preventing, maximizing healthy years. It's time to pay attention to the subtle messages your body is sending, because AI is finally learning to listen.


