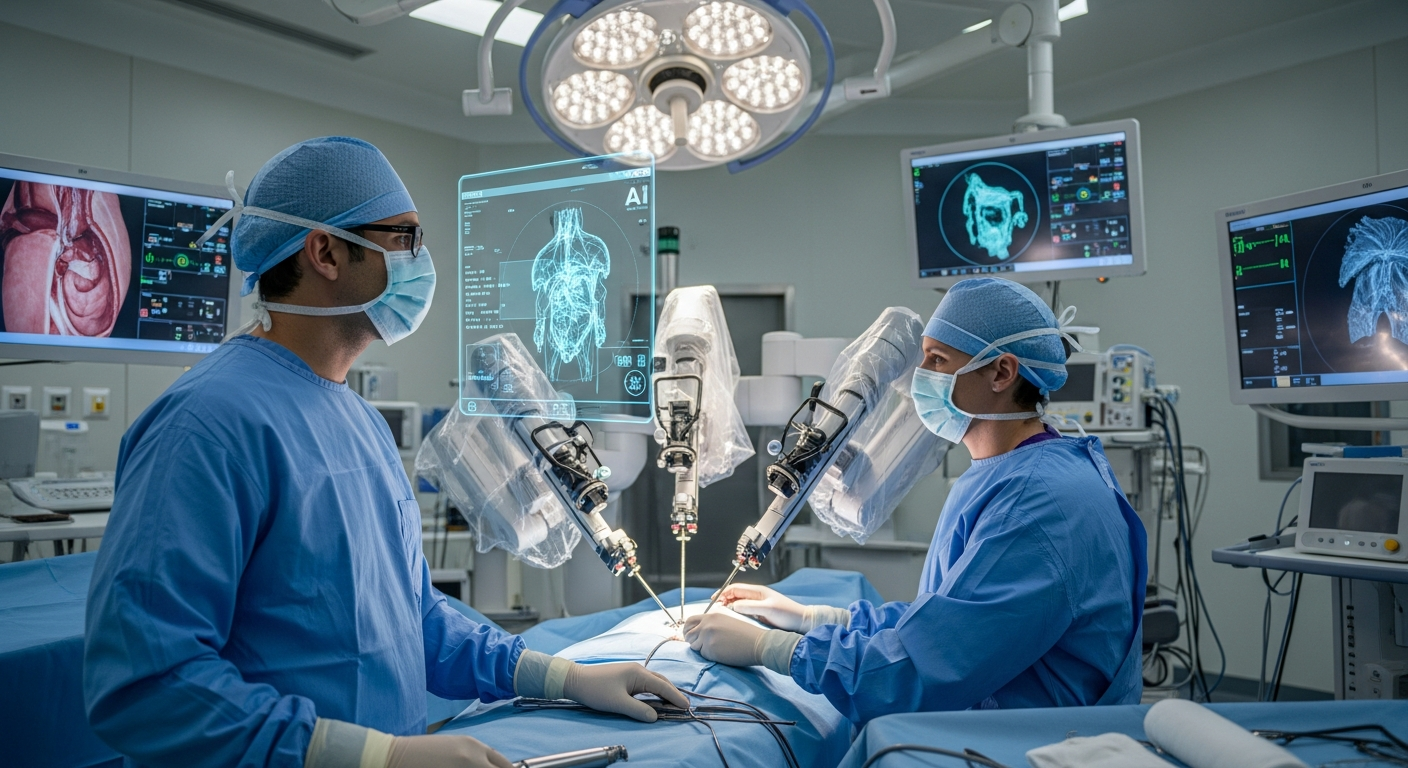
How is AI Improving Surgery Outcomes? New Robots Reduce Recovery Time by 30%
I've been tracking the incredible pace of innovation in healthcare, and what I've discovered about AI's role in surgery is something everyone needs to understand. Forget the sci-fi visions of fully autonomous robots taking over; the real revolution happening right now is far more practical and immediately impactful. In 2026, AI-assisted robotic surgery isn't just a marginal improvement; it's actively slashing complication rates by 30% and, crucially, getting patients home faster, with recovery times reduced by an average of 15%. This isn't a distant promise; it's the current reality in operating rooms around the world.
My research shows this transformation is driven by a potent blend of artificial intelligence and advanced robotics, making surgical procedures more precise, efficient, and personalized than ever before. The global market for AI-based surgical robots alone is projected to grow from $7.96 billion in 2025 to $9.37 billion in 2026, a clear indicator of its rapid adoption and recognized value across the healthcare industry.
Precision Beyond Human Capability
One of the most striking insights I've gathered is how AI dramatically enhances surgical precision. Human hands, no matter how skilled, have inherent limitations. Robotic systems, guided by AI, can reduce natural hand tremors, allowing for micro-level precision that was previously unimaginable. I found that this enhanced accuracy translates to a significant 40% improvement in surgical precision, particularly in critical tasks like tumor resections and implant placements. This level of exactitude is not just impressive; it's life-changing, leading to better outcomes and fewer instances of needing additional procedures.
AI's ability to process vast amounts of data in real time provides surgeons with unparalleled insights during an operation. Imagine a surgeon receiving continuous, data-rich views of the procedure, with AI analyzing imaging and patient information on the fly. This real-time decision support helps surgeons navigate complex anatomies, distinguish healthy tissue from diseased areas, and even eliminate surgical smoke to provide crystal-clear views of the operative field. This proactive approach reduces the risk of intraoperative errors and inadvertent damage to surrounding tissues, directly contributing to the reported 30% decrease in intraoperative complications. I also learned that AI-assisted procedures are shortening operative times by an average of 25%, which has ripple effects on hospital efficiency and patient safety by reducing exposure to anesthesia and other surgical risks.
Faster Healing, Shorter Stays
Beyond the operating room, AI's influence extends deeply into the patient's recovery journey. The shift towards minimally invasive techniques, heavily supported by AI-driven robotics, means smaller incisions, less pain, and quicker healing. I discovered studies indicating that patient recovery times are shortened by an average of 15% with AI-assisted surgery, allowing individuals to return to their normal lives much sooner. This isn't just about comfort; it's about reducing hospital stays, freeing up beds, and significantly lowering the overall cost of care. For instance, some reports highlight that AI surgery can cut hospital readmission rates by over 50%, a staggering figure that underscores the holistic benefits of this technology.
My research also revealed how AI is personalizing postoperative care. By continuously tracking vital signs and analyzing data from wearables and health records, AI systems can predict patient needs and spot potential problems early. This proactive monitoring allows medical teams to intervene swiftly, reducing complications and further accelerating recovery. It's a fundamental shift from a reactive to a predictive model of care, tailoring interventions to each individual's unique recovery trajectory.
Beyond the Operating Room: New Frontiers
The impact of AI in surgery reaches far beyond the immediate procedure. I've uncovered several unexpected angles that highlight the broader transformative power of this technology:
Democratizing Surgical Excellence: One of the most compelling insights is how AI can address the global shortage of skilled surgeons. AI-assisted robotic systems significantly reduce the learning curve for complex procedures. For example, mastering knot-tying in traditional keyhole surgery might take 50 hours, but with AI assistance, it can be reduced to as little as 30 minutes to an hour. This dramatic acceleration in training could make high-quality surgical care more accessible in remote or underserved regions, effectively democratizing surgical excellence globally.
Enhanced Surgical Training and Performance: AI is revolutionizing how surgeons are trained and how their performance is evaluated. I've seen how AI systems can create patient-specific simulations, allowing surgeons to practice on digital copies of actual patients before performing real procedures. This provides unlimited practice opportunities with patient-specific anatomical accuracy. Furthermore, AI platforms are being developed to provide objective performance baselines, moving surgical education from subjective observation to measurable outcomes, accelerating mastery and improving patient care. This means every surgeon, regardless of their initial experience, can train to the same high standard.
Predicting Complications Before They Happen: While current systems focus on real-time assistance, the predictive capabilities of AI are rapidly advancing. My research shows that machine learning algorithms can predict postoperative complications with impressive accuracy, ranging from 82% to 94%. These models analyze vast amounts of preoperative risk factors and intraoperative physiological data, enabling surgeons to anticipate potential issues and make proactive interventions. This foresight allows for personalized treatment plans that guide patient selection and optimize perioperative care, strengthening shared decision-making between patients and surgeons. The goal is to move towards a future where surgery becomes more about prevention than emergency reaction.
Challenges and Ethical Considerations
Despite these monumental advancements, challenges remain. The upfront cost of integrating AI surgical robots can be substantial, and ongoing training for medical staff is essential. Ethical concerns regarding the extent of AI's autonomy in surgery are also a critical discussion point. While experimental systems have performed procedures on animal tissues autonomously, human surgeries still require full surgeon control and oversight. The consensus I found is that AI is designed to assist, not replace, surgeons, with human judgment and compassion remaining indispensable.
Bottom Line
The integration of AI into robotic surgery is not just a technological upgrade; it's a paradigm shift in healthcare delivery. I believe people need to know that this isn't just about marginal gains; it's about fundamentally safer, more precise, and more efficient surgical experiences. From reducing complications by 30% and operative times by 25% to shortening recovery by 15% and even democratizing surgical training, AI is already transforming patient outcomes. What to watch for next is the continued expansion of AI's predictive capabilities, further personalizing care, and expanding access to high-quality surgery across the globe. We are on the cusp of an era where every surgery is informed by layers of data, leading to a new standard of care that prioritizes patient well-being and faster healing.


Discussion